Achilles Tendonitis
Achilles Tendonitis is a condition that occurs when the Achilles Tendon, the large tendon that runs down the back of your lower leg, becomes irritated and inflamed. Causes for inflammation of the Achilles Tendon include repetitive overuse and degeneration of the tendon as micro-tears develop and may alter the structural makeup of the tendon. Cases of Achilles Tendonitis can range from relatively mild to severe. Mild cases can typically be treated with relatively simple, at-home care under your doctor’s supervision. Meanwhile, moderate to severe cases may require further medical attention in order to achieve resolution of symptoms. In addition, self-care strategies such as stretching and strengthening, as well as preventive measures such as selecting proper footwear and avoiding sudden excessive increase in volume of physical activity without gradual build-up in tolerance are usually necessary to prevent recurring episodes.
Symptoms:
- Pain and stiffness along Achilles Tendon that worsens with physical activity
- Swelling that is present all the time and worsens throughout the day with physical activity
- Tenderness upon palpation of tendon
- Thickening of the tendon
- Severe pain the day following exercise
When to see a Specialist
If you experience persistent pain around the Achilles tendon which is limiting your daily activities, call your doctor for an assessment. Seek immediate medical attention if the pain or disability is severe. Prolonged Achilles Tendonitis without proper medical attention may lead to weakening of tendon and may result in having a torn (ruptured) Achilles tendon.
Acute care
With initial onset of pain it is important to avoid causing more irritation and inflammation by avoiding activities that cause increase in symptoms. To try to help reduce symptoms and manage pain with some self- care tactics that can be used are resting, using ice, compression wraps and elevation.
-Rest: By resting you can allow symptoms to reduce and prevent causing further damage and inflammation to the tendon
-Ice: Ice for 15 to 20 minutes can help reduce inflammation and decrease the pain. Ice can be used multiple times a day.
-Compression: Utilizing compression with an ace wrap or compression sleeve is beneficial to reduce swelling and provide stability for the injured area.
-Elevation: Elevating the ankle above the heart can help with reducing inflammation. Elevation in conjunction with ice can help further reduce inflammation
Exercises
There are many exercises that can help improve achilles tendonitis, these exercises consist of both stretching and strengthening. These exercises can be performed 2 to 3 times a day and with consistency can help with improving active mobility and flexibility of the ankle.
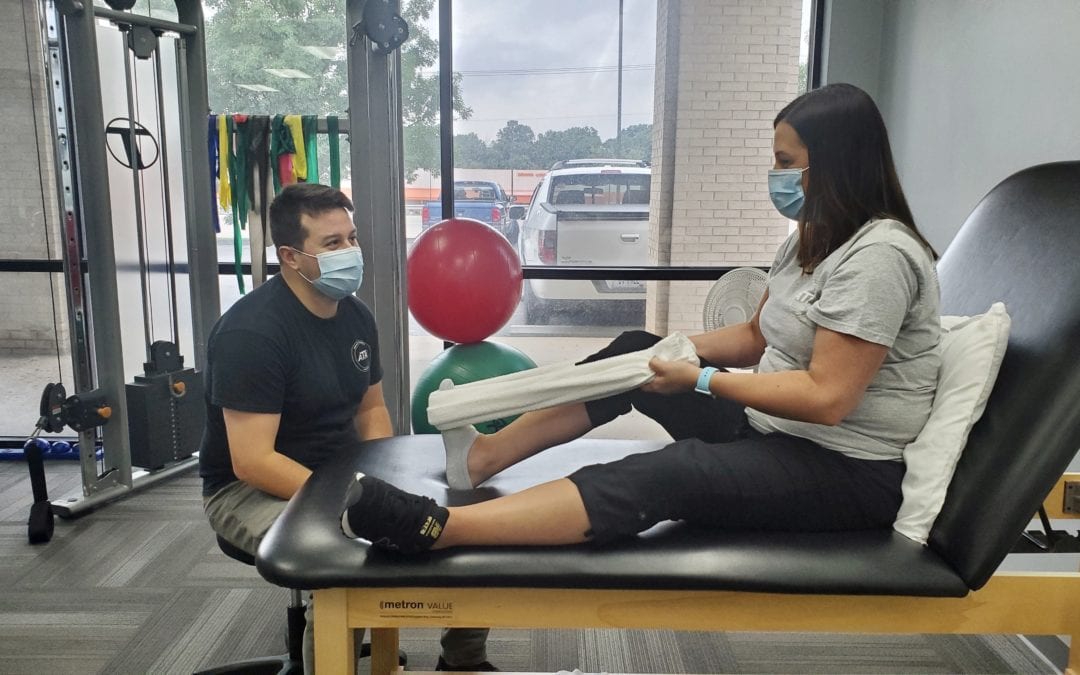
Towel stretch with knee at full extension
This is done by using a towel and placing the towel along the ball of the foot with a fully extended knee and pulling the foot toward the upper body until a gentle stretch is felt in the back of the calf, hold stretch for about 10 seconds and repeat 15 times. This stretch will target the gastroc-soleus complex which makes up the back of the calf.

Towel stretch with knee bent
This is done by using a towel and placing the towel along the ball of the foot with a bent knee and pulling the foot toward the upper body until a gentle stretch is felt in the back of the calf, hold stretch for about 10 seconds and repeat 15 times. This stretch will target the soleus which helps make up the posterior calf.



Ankle alphabet
Without using your upper leg or hip you will use the ankle to draw the letters of the alphabet, both upper and lower case, perform 2 sets twice daily. While performing this exercise you should go slow and controlled to allow all muscles to activate properly.
How can Physical Therapy help?
Physical Therapy can improve symptoms of Achilles Tendonitis including swelling, range of motion, strength and balance deficits. Physical Therapists (PTs) and Physical Therapist Assistants (PTAs) can use a variety of interventions to address these symptoms including, but not limited to: modalities (cold pack, ultrasound, electrical stimulation), stretches, strengthening exercises, balance techniques, and manual therapy (soft tissue massage, passive range of motion). Your therapist may also suggest the use of orthotics or more supportive shoewear in conjunction with the interventions provided in Physical Therapy. It can be expected to work with your individual healthcare team and utilize a variety of tools to return to your desired activities!
The ultimate goal is to help you understand the best strategies to manage your symptoms and get you back to your desired activities!
Authors: Deanna Grommet, PTA, Jordan Verbanaz, DPT