
May is National Arthritis month!
Arthritis is one of the most common diagnoses we treat in Physical Therapy and cases are only expected to increase over the next 10 years. There are many types of arthritis and knowing how to manage a new diagnosis can be overwhelming. Here is everything you need to know about the most types and management of adult arthritis.
Three Most Common Types
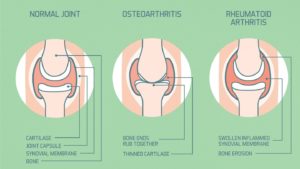
Osteoarthritis or OA is the most common form and oftentimes affects the larger weight bearing bones in the body including the hip and knee. It can be referred to as “bone on bone” because it is characterized by the wearing down of cartilage on the ends of two bones comprising a joint. Pain is felt as friction increases when the bones rub against each other.
Rheumatoid Arthritis or RA is an auto-immune disease in which the body’s inflammatory response kicks in and attacks the lining of joints. A very common area for this to occur is within the small joints of the hand.
Psoriatic Arthritis is one that affects both the skin as well as the joints. It is linked to the diagnosis of psoriasis. People will often present with red scaly rashes on their skin as well as swelling present within the joints under the skin. It is also very common in the hand as well as in the toes.
Diagnosis
Diagnosis of OA, RA, and Psoriatic Arthritis can be made by a physician following a full systems review, physical exam, imaging including X-rays, and lab work. Oftentimes, a consultation to a Rheumatologist can be made in order to ensure proper diagnosis of Rheumatoid as well as Psoriatic Arthritis.
Treatment Options
OA treatment options include conservative treatment as well as surgical treatment. Conservative treatment for OA includes utilizing braces as well as assistive devices in order to offload the joint when moving throughout the day. Physical therapy can be prescribed in order to strengthen the muscles surrounding the joint as well as to provide education to patients about how to safely increase physical activity levels. Surgical treatment of OA most likely will include either an arthroscopic surgery, an osteotomy, a joint fusion, or a joint replacement. Following surgical interventions, physical therapy can be prescribed to improve joint mobility, increase muscle strength, and assist a patient in returning to full independence with all their daily activities.
Treatment of RA includes use of medications as well as learning self-management strategies to improve pain level and function with daily activities. DMARDs (disease-modifying antirheumatic drugs) and biological response modifiers are two examples of medications utilized to slow the progression of RA and also prevent joint deformity. Self-management strategies can include weight loss as well as improving physical activity levels. Physical Therapy treatment to improve joint mobility, improve muscle strength, and provide education on proper physical activity levels can be beneficial to many people diagnosed with RA.
Psoriatic Arthritis treatment includes both skin and joint interventions. Possible medications utilized to treat Psoriatic Arthritis include Non-steroid anti-inflammatory medications, corticosteroids, and immunosuppressive medications such as methotrexate. Physical Therapy and Occupational Therapy can both be beneficial to treatment of psoriatic arthritis in order to improve muscle function as well as joint mobility.
Everyone’s symptoms will vary with these types of arthritis, but one thing we know is that it doesn’t have to slow you down! Millions of people worldwide continue to live active, fulfilling lives managing their symptoms. Physical Therapy is a key treatment for any type of joint related arthritis to maintain the mobility and strength needed to complete your desired tasks.
Patient-centered individualized Physical Therapy treatment at ATR can help you to manage your symptoms and get back to the activities you love!
Author: John Cichon, PT DPT



